Treating Disruptive Behavior Disorders in Children
 Child & adolescent psychiatrist; medical director, child & youth mental health services at Lady Cilento Children’s Hospital, Brisbane, Australia; senior lecturer, University of Queensland, visiting senior lecturer, Flinders University Dr. Parry has disclosed that he has no relevant financial or other interests in any commercial companies pertaining to this educational activity.
Child & adolescent psychiatrist; medical director, child & youth mental health services at Lady Cilento Children’s Hospital, Brisbane, Australia; senior lecturer, University of Queensland, visiting senior lecturer, Flinders University Dr. Parry has disclosed that he has no relevant financial or other interests in any commercial companies pertaining to this educational activity.
CCPR: Dr. Parry, what sort of experience do you have working with children with disruptive behavioral disorders (DBDs)?
Dr. Parry: Beyond 20 years of general child psychiatrist clinical experience, my current role is with a preadolescent child and family inpatient unit in a large pediatric hospital in Brisbane, Australia, where we specialize in disruptive behavior disorders.
CCPR: When people talk about disruptive disorders, what does that include?
Dr. Parry: In DSM terms, attention-deficit/hyperactivity disorder (ADHD), oppositional defiant disorder (ODD), and conduct disorder (CD). But, in practice, also comorbidities with autistic spectrum disorders (ASD), learning disorders (LDs), speech and language delays, attachment problems, developmental trauma, ongoing maltreatment, and family and school dynamics abound. Puberty often exacerbates disruptive behavior—even in normal children—let alone when there are other factors. Disruptive mood dysregulation disorder (DMDD) does not seem to be used in Australia, perhaps because pediatric bipolar disorder (BD) in children was never widely used either. Also, the Australian public health system uses ICD-10 codes, which don’t include DMDD. Funding is not directly tied to diagnostic labels in public or private health systems, so usually the focus is on a biopsychosocial diagnostic formulation rather than a specific diagnosis. Educational and welfare funding is tied to ASD diagnoses, and there is debate about overdiagnosis of ASD.
CCPR: How common are these disorders?
Dr. Parry: The DBDs are the most common preadolescent disorders in child psychiatry and behavioral pediatrics. In our unit, we have many pre-pubertal children with an array of oppositional, defiant, conduct, and inattention symptoms who may or may not be mildly to severely autistic. These children display highly disruptive behaviors. At the point we see them, their parents or foster caregivers cannot manage them, and their treating pediatricians, psychiatrists, and mental health services have reached some kind of impasse. They are often taking a considerable cocktail of medications. They come to us for diagnostic clarification and to review their medication regimens.
CCPR: How old are the children you’re working with?
Dr. Parry: We take kids starting at around age 5 up to late puberty, including developmentally “younger” 14-year-olds. We have some capacity to admit parents along with the child to work on parenting and family aspects.
CCPR: Could you talk a little bit about your sense of how disruptive disorders evolve with different age groups like the preschoolers, school age, early teens, and then adolescents?
Dr. Parry: In terms of inpatient child and adolescent psychiatry, the preschool- and school-age groups are mostly boys and some girls with the mixture of comorbidities I mentioned. With regard to our adolescent inpatient unit, there are two main groups: one involves suicidal risks and borderline personality dynamics, usually from an environment of trauma; the second is individuals with emerging and manifest psychosis.
CCPR: In the U.S., we would add to that CD kids, who certainly are in the disruptive disorder category but don’t quite fit into any of those you just mentioned.
Dr. Parry: We do have them in our child unit. But, in an adolescent inpatient setting, they can quickly disrupt the therapeutic milieu, so we endeavor to discharge them as soon as a brief suicidal crisis, sometimes with substance intoxication (the most likely reason for admission), has settled. We do have a trauma-informed forensic adolescent service to refer them to, particularly in the youth detention centers if they’ve been sentenced, but there is a need for more forensic adolescent resources.
CCPR: How do you go about diagnosing DBD in kids?
Dr. Parry: Our model is to focus on creating a full diagnostic biopsychosocial formulation. This requires a thorough developmental history, including a trauma history if relevant. We look at school guidance testing and psychometrics testing such as the Wechsler Intelligence Scale for Children (WISC). We have a speech pathologist on our unit and often find a speech and language assessment is valuable, because many of these children don’t have the language they need to understand or to express their emotions. We do ADHD scales as well and are fortunate to have a hospital school that provides further input from teachers. In community clinics, it can be too easy to make an ADHD diagnosis based on limited information from the parents and the behavior of the child in your office, which may not be typical of their overall behavior.
CCPR: How does this individualized approach help you plan treatment?
Dr. Parry: Once we have a comprehensive diagnostic formulation, the management plan becomes self-evident. You can see what proportion is medication oriented; what proportion is helping this child deal with perhaps more recent discrete loss or trauma through some psychotherapy; what proportion is child abuse and neglect, requiring us to notify child protection to assess whether the child is safe to return to his or her place of residence; what proportion warrants—and this is common—parent training or family therapy. Then we try to initiate the interventions their formulation suggests will be most helpful, while passing the diagnostic formulation on to their community-based clinicians for ongoing therapy.
CCPR: What medications do you find useful?
Dr. Parry: If we have a child who meets criteria for ADHD, we’ll try the stimulants in the inpatient environment; but, if the behavior has anxiety inputs from stress and trauma and a child does not actually have the genes or early neurodevelopment adversity that would have led to a more biological ADHD, we often find that stimulants don’t do much.
CCPR: What about other drugs such as antidepressants, anticonvulsants, and antipsychotics?
Dr. Parry: A lot of children these days in Australia are on SSRIs and antipsychotics, as is true also in the U.S. Very few are on anticonvulsants, unless they have epilepsy or are older adolescents with well-established manic episodes. Personally, I’ve only seen benefit using SSRIs with the DBDs if there’s a significant anxiety or obsessive-compulsive component that’s driving the disruptive behavior. I think SSRIs are overused particularly in milder adolescent depression. Consistent with the research, I’ve seen a number of adolescents develop increased suicidality, and their prescriber had oftentimes not warned them or parents of the risk. I also find the long-term risks of antipsychotics concerning.
CCPR: Can you elaborate?
Dr. Parry: Sure. Undoubtedly the antipsychotics do dampen severe disruptive behavior and may address sensory hypersensitivity as a core problem in autism. However, there is research by Nancy Andreason and colleagues on adults with schizophrenia that suggests that there is some degree of neuronal atrophy from many years of antipsychotics despite the fact they are necessary in suppressing psychotic symptoms (Ho BC et al, Arch Gen Psychiatry 2011;68:128–137). Unfortunately, the studies haven’t been done to say what it means to the growing brain to be on risperidone for many years. Could it cause future neuronal atrophy, so that the child never reaches full cognitive potential? That’s concerning to me. And that’s not including the extrapyramidal side effects. One study suggests that second-generation antipsychotics (SGAs) cause fewer extrapyramidal side effects, but they still found a 6% rate of tardive dyskinesia (TD) in children and adolescents after 6 months (Wonodi et al, Mov Dis 2007;22(12):1777–1782). Given the scale of off-label prescribing, possible TD in children is a subject calling out for more research.
CCPR: What about metabolic syndrome?
Dr. Parry: That’s a big one. We get children who have packed on so much weight that they are throwing their weight around, literally: Patients who could previously restrain them can’t do so anymore, so the child ends up in an inpatient unit.
CCPR: That’s understandably worrisome. Any other medications you can speak to?
Dr. Parry: We use clonidine. It’s an old-fashioned, cheap drug. It suppresses the epinephrine rather than the dopaminergic neural networks, and it has a sedating effect and may reduce oppositional behavior. It’s also theorized to have a stimulating effect on the prefrontal cortex that may help ADHD. Of course, it’s risky in terms of overdose, and we are careful that the parents fully understand this and lock it away. It can replace an antipsychotic or at least allow for antipsychotic dose reduction. Similarly, in the inpatient setting, we use benzodiazepines, mainly lorazepam, for as-needed sedation. We very rarely see children who become paradoxically agitated on benzodiazepines. But benzodiazepines have problems of tolerance and lose effectiveness for long-term use at home, though judicious dispensing by capable parents can work in some cases.
CCRP: It sounds like, at least in your setting, that you try to use medication quite judiciously. I would assume there are kids coming in for whom others have used them less selectively. How does it work in terms of keeping kids on or taking them off prior medication?
Dr. Parry: We try to take them off as best we can. Sometimes, we don’t make much headway, particularly with children with more severe ASD. But, in other cases, the combination of parent training and self-regulation strategies for the child allow for medication dose reductions.
CCPR: How do you teach self-regulation strategies?
Dr. Parry: On our child inpatient unit, we talk about basic neurophysiology with children and parents and explain things like sympathetic (“S for Stress”) fight/flight/freeze responses versus parasympathetic (“P for Peace”) “rest/digest/grow” nervous systems. Then we explain how diaphragmatic breath control via vagus nerve stimulation as in yawning, sighing, laughing, and yoga “ujjayi” (Sanskrit for “victory”) breaths, as well as attachment security as in calm parental voice, triggers the peaceful parasympathetic system. Thus, children and parents gain an empowering understanding of their own hard-wired instinctive circuit breaker to induce relaxation and reduce anger and anxiety of fight/flight. We’ve also recently introduced some biofeedback computer games that work on heart rate variability to entrain engagement of the “peaceful” parasympathetic system.
CCPR: You mentioned parent training as well. What is your approach to that?
Dr. Parry: Before we introduce new skills, it’s essential to be empathic with the parents, so they understand we are in no way criticizing them. One specific technique we use is the “Triple-P” parent training program.
CCPR: What does Triple-P stand for?
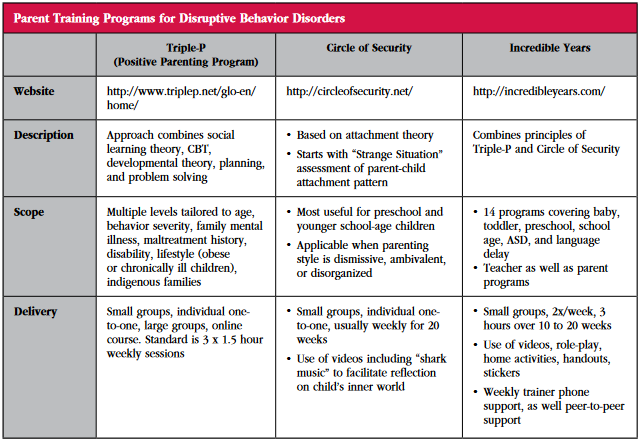
Dr. Parry: It stands for Positive Parenting Program, and it is a behaviorist approach that is evidence based. It was developed at the University of Queensland by Professor Matthew Sanders, and it’s now used in 25 countries. There are various modules for teaching parenting skills for preadolescents, teens, children with disabilities, families in divorce situations, etc. The basic premises are creating a safe and interesting environment for your child, positive reinforcement of pro-social behavior, clear rules, distraction, planned ignoring, fair consequences, and parental self-care (for quick summaries on Triple-P and other parent training programs see the table).
CCPR: Sounds like a solid approach. I assume there are other types of disruptive behavior patterns that are even more entrenched and challenging for families.
Dr. Parry: Yes. A lot of the families that we see have problems that run deep—such as insecure attachment that affects the child’s basic trust. In these cases, we add Circle of Security parent training, which has a smaller research base than Triple-P, though that is growing. The concepts are nicely delivered for parents, and it is becoming popular.
CCPR: What is the Circle of Security?
Dr. Parry: It’s a psychoeducational model for helping parents understand the importance of secure attachment with their children while also giving their children some space. It was developed by a group of clinicians in Spokane, WA, and has its roots in John Bowlby’s attachment theory and Donald Winnicott’s idea of the “holding space.” Circle of Security includes the concept of “shark music.” Parents are shown a video of a child walking along a path towards the beach, and there’s this lovely music playing. And they think, “Oh, this child is going to the beach,” and this evokes a good feeling about the child having a fun day at the beach. Then the same visual is replayed, but the music changes to menacing—the Jaws theme, aka shark music—and now the feeling is “Oh, something dreadful is going to happen.” This technique helps parents emphasize with what’s going on in the child’s mind. How might the shark music trigger an aggressive loss of temper in your child? Where is the shark music in the child’s mind? Where is the shark music in your mind? The program also includes a “circle of repair” to help parents in healing the attachment ruptures with their children.
CCPR: That’s very interesting. Thank you for your time, Dr. Parry.
Newsletters
Please see our Terms and Conditions, Privacy Policy, Subscription Agreement, Use of Cookies, and Hardware/Software Requirements to view our website.
© 2026 Carlat Publishing, LLC and Affiliates, All Rights Reserved.


_-The-Breakthrough-Antipsychotic-That-Could-Change-Everything.webp?t=1729528747)



