Home » Vitamin D for ADHD?
Vitamin D for ADHD?
October 30, 2020
From The Carlat Child Psychiatry Report
Kristen Gardner, PharmD.
Dr. Gardner has disclosed that she has no relevant financial or other interests in any commercial companies pertaining to this educational activity.
Review of: Gan J et al, J Child Adolesc Psychopharmacol 2019;29(9):670–687
Many children do not respond to or tolerate standard pharmacotherapy, which drives continued interest in supplements for many conditions, including ADHD. Vitamin D plays a role in healthy brain development, and vitamin D deficiency causes neurotransmitter alterations in pathways underlying ADHD pathogenesis. But is there a link between ADHD and lower vitamin D levels? These researchers conducted a systematic review and meta-analysis to assess the strength of evidence to date.
The study looked at four randomized controlled trials (n = 256) studying vitamin D supplementation for ADHD (1,000 international units [IU] daily–50,000 IUs weekly) vs placebo as adjunctive to methylphenidate for children (5–18 years). Trial durations lasted 6–12 weeks. The researchers assessed ADHD symptom severity level based on a variety of parent-only rating scales as the primary outcome. The secondary outcomes were adverse effects of supplementation and vitamin D status afterwards.
Adjunctive vitamin D supplementation yielded a small but statistically significant improvement in ADHD total score and inattention, hyperactivity, and behavior subscales. Scores for oppositional behaviors were unchanged except in a subgroup analysis of high-dose vitamin D supplementation (> 2,000 IUs daily). Notably, one study found that children with baseline vitamin D deficiency or insufficiency were more likely to respond to adjunctive vitamin D supplementation. Only one trial reported on adverse events, which were mild and similar between groups. Not surprisingly, vitamin D supplementation increased vitamin D levels and also increased the ratio of patients with sufficient vitamin D levels.
This paper used excellent methodological procedures for conducting systematic reviews and meta-analyses. Unfortunately, the RCTs were of very low to low quality. Randomization procedures were not clear, the total population was less than 400, and statistical methods varied. All of these trials were carried out in the Middle East, but children’s ethnicities were not reported, so generalizability is unclear.
CCPR’s Take
Vitamin D supplementation is a relatively low-risk and low-cost intervention with general health benefits. We recommend you consider trying it both in children with vitamin D deficiency and in combination with standard ADHD treatment. It’s unclear whether similar results would extend to non-methylphenidate stimulants. More research is needed using higher-quality evidence that examines whether vitamin D dose, administration frequency, and baseline status influences outcomes. Do take care to avoid mega-doses, though, as this can disrupt calcium metabolism.
Child PsychiatryMany children do not respond to or tolerate standard pharmacotherapy, which drives continued interest in supplements for many conditions, including ADHD. Vitamin D plays a role in healthy brain development, and vitamin D deficiency causes neurotransmitter alterations in pathways underlying ADHD pathogenesis. But is there a link between ADHD and lower vitamin D levels? These researchers conducted a systematic review and meta-analysis to assess the strength of evidence to date.
The study looked at four randomized controlled trials (n = 256) studying vitamin D supplementation for ADHD (1,000 international units [IU] daily–50,000 IUs weekly) vs placebo as adjunctive to methylphenidate for children (5–18 years). Trial durations lasted 6–12 weeks. The researchers assessed ADHD symptom severity level based on a variety of parent-only rating scales as the primary outcome. The secondary outcomes were adverse effects of supplementation and vitamin D status afterwards.
Adjunctive vitamin D supplementation yielded a small but statistically significant improvement in ADHD total score and inattention, hyperactivity, and behavior subscales. Scores for oppositional behaviors were unchanged except in a subgroup analysis of high-dose vitamin D supplementation (> 2,000 IUs daily). Notably, one study found that children with baseline vitamin D deficiency or insufficiency were more likely to respond to adjunctive vitamin D supplementation. Only one trial reported on adverse events, which were mild and similar between groups. Not surprisingly, vitamin D supplementation increased vitamin D levels and also increased the ratio of patients with sufficient vitamin D levels.
This paper used excellent methodological procedures for conducting systematic reviews and meta-analyses. Unfortunately, the RCTs were of very low to low quality. Randomization procedures were not clear, the total population was less than 400, and statistical methods varied. All of these trials were carried out in the Middle East, but children’s ethnicities were not reported, so generalizability is unclear.
CCPR’s Take
Vitamin D supplementation is a relatively low-risk and low-cost intervention with general health benefits. We recommend you consider trying it both in children with vitamin D deficiency and in combination with standard ADHD treatment. It’s unclear whether similar results would extend to non-methylphenidate stimulants. More research is needed using higher-quality evidence that examines whether vitamin D dose, administration frequency, and baseline status influences outcomes. Do take care to avoid mega-doses, though, as this can disrupt calcium metabolism.
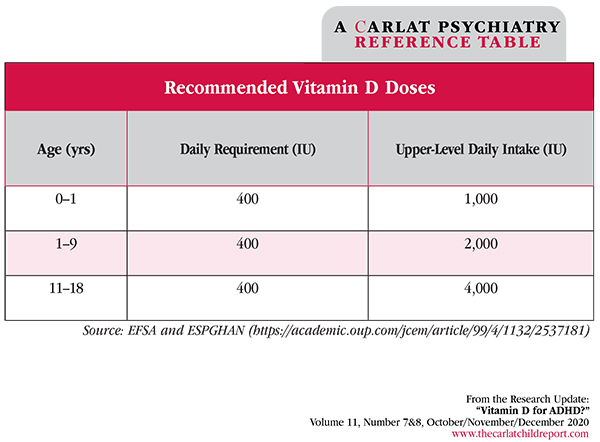
Table: Recommended Vitamin D Doses
(Click to view full-size PDF.)
Issue Date: October 30, 2020
Table Of Contents
Recommended
Newsletters
Please see our Terms and Conditions, Privacy Policy, Subscription Agreement, Use of Cookies, and Hardware/Software Requirements to view our website.
© 2026 Carlat Publishing, LLC and Affiliates, All Rights Reserved.


_-The-Breakthrough-Antipsychotic-That-Could-Change-Everything.webp?t=1729528747)



