Herbal Therapies for Depression

 Scott Mendelson, MD, PhD.
Scott Mendelson, MD, PhD.
Recently retired after 25 years of practicing inpatient and outpatient psychiatry in community and VA hospitals. He is the author of several psychiatric textbooks including Herbal Treatment of Major Depression (CRC Press, 2019) and Herbal Treatment of Anxiety (CRC Press, 2022).
Dr. Mendelson has no financial relationships with companies related to this material.
TCPR: What is the difference between a drug and an herb?
Dr. Mendelson: There really is no difference in terms of their pharmacological actions. A lot of medications are derived from plants and then altered to make them more potent, lipophilic, or resistant to enzymatic breakdown. For example, the acetyl groups are added to salicylate from willow to make aspirin or to morphine from poppies to make heroin, but the underlying mechanisms of action are the same. In psychiatry, valproate is a methylated derivative of valeric acid from valerian root, bupropion is a derivation of cathionine from the khat plant, and galantamine (used to treat dementia) is found in pure form in the bulb of the snowdrop plant.
TCPR: But herbs contain many chemicals while medications have only one.
Dr. Mendelson: Yes, that may be the more important difference. In Western medicine, we look for the single silver bullet and polypharmacy is discouraged. But every herb contains dozens of phytochemicals. In the Chinese and Ayurvedic (Indian) traditions, these various phytochemicals are thought to act synergistically, even though one may have the primary effect.
TCPR: How are herbal capsules different from the natural form of the plant?
Dr. Mendelson: Herbs are sold as purified, standardized, or full spectrum. Purified is when the phytochemical that is thought to produce the desired effect is isolated, such as hypericin from St. John’s wort. In standardized products, the extract is adjusted to contain a specific concentration of the active phytochemical, such as St. John’s wort with 0.3% hypericin. Full-spectrum extracts are not adjusted. They are simply aqueous or alcoholic extracts of the plant that contain the full range of phytochemicals, each of which may contribute to the therapeutic effect in subtle ways.
TCPR: Which is better?
Dr. Mendelson: If positive studies used isolated or standard extracts, then it’s probably wise to use the same in treatment. However, herbalists prefer full-spectrum extracts. That is how humankind discovered the benefits of plants in the first place, and that is how they have been used for centuries. This is a controversial area, and we don’t have clear studies showing that one way is better than the other.
TCPR: Some patients view herbs as natural, but they aren’t natural to the human body like folate or omega-3s are.
Dr. Mendelson: That is partly true. On the other hand, we have evolved alongside these plants, and humans have a much longer history of consuming them than they do industrial medicines. For example, flavonoids are a common therapeutic ingredient in herbal medicine. Flavonoids are found in all plant-based foods. Several epidemiologic studies have found an association between higher levels of flavonoid consumption and lower rates of depression, though these don’t prove causation (Bardinet J et al, Clin Nutr 2022;41(12):2628–2636). So herbs may serve a natural restorative function in maintaining health as opposed to simply treating disease.
TCPR: Do herbal compounds bring new mechanisms to the table?
Dr. Mendelson: Yes, and again flavonoids are a good example. There are over 1,800 varieties of flavonoids and all herbal therapies have them. They address the pathophysiology of depression in ways that antidepressants do not, such as improving mitochondrial and metabolic function or reducing oxidative damage and inflammation. They have neuroprotective effects. Flavonoids also have pharmacodynamic effects that overlap with medications, such as at the GABA-A receptor that benzodiazepines act on, reversible MAO inhibition, or signaling cascades that are involved in ketamine’s mechanism of action (like mTOR, MAP kinases, and glycogen synthase kinase). Flavonoids are not the only active ingredient in herbal therapies. Other herbs to consider are adaptogens.
TCPR: What is an adaptogen?
Dr. Mendelson: The word was coined by a Russian physiologist who saw that certain herbs built stamina and resiliency against stress. Examples are ashwagandha, ginseng, Rhodiola rosea, and water hyssop (aka brahmi). Many of these contain steroid-like phytochemicals. They buffer the effects of glucocorticoids, which are released in excess under stress. With chronic stress, the brain and body develop resistance to high levels of glucocorticoids, and adaptogens modify that effect.
TCPR: Which herbs have the best evidence in depression?
Dr. Mendelson: St. John’s wort, saffron, and turmeric (usually taken as its active extract, curcumin). The one with the strongest evidence is St. John’s wort, with 27 clinical trials involving 3,808 subjects in the latest meta-analysis (Ng QX et al, J Affect Disord 2017;210:211–221). Their conclusion was that St. John’s wort is comparable in efficacy to SSRIs but with fewer side effects. However, there have been negative studies, and St. John’s wort is not very effective for severe depression. Its mechanism of action is still not entirely clear, but it seems to decrease reuptake of monoamines and other neurotransmitters.
TCPR: What are the risks with St. John’s wort?
Dr. Mendelson: Like antidepressants, it can cause hypomania. Like tricyclics, it can cause photosensitivity. But the biggest concern is drug interactions. St. John’s wort can lower levels of many medications, including birth control pills and HIV medications, because it is a strong inducer at CYP enzymes (particularly 3A4, but also 1A2, 2C9, and 2C19). That interaction takes place in the liver, but St. John’s wort also induces P-glycoprotein at the blood-brain barrier, which makes it difficult for many antidepressants and a few antipsychotics to get into the brain. Finally, it can cause serotonin syndrome with MAOIs, SSRIs, SNRIs, and MAOIs. I don’t use it with other psychiatric medications.
TCPR: Any advice on choosing a product?
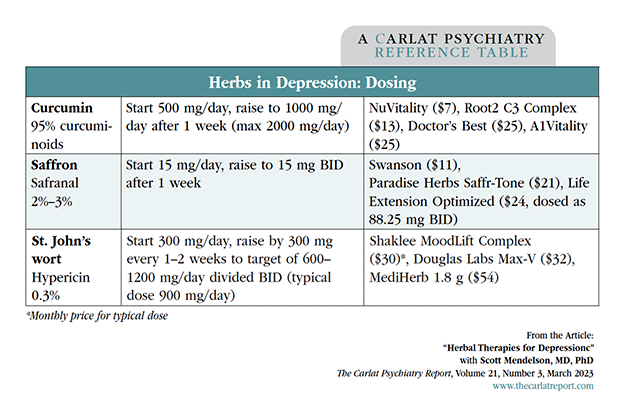
Dr. Mendelson: You have to be careful with St. John’s wort because most products—around 40%–60%—don’t have as much of the active ingredient as they say they do (Frommenwiler DA et al, J AOAC Int 2016;99(5):1204–1212). The brand I prefer is Douglas Labs because it has both standardized and full-spectrum components. That way you get the research-based dose of hypericin, along with the other subtle components that are known to have antidepressant effects as well (Editor’s note: See the table “Herbs in Depression: Dosing”). I divide the dose twice a day and give the larger portion at night because it can help with sleep.
TCPR: Tell us about turmeric.
Dr. Mendelson: Turmeric is a member of the ginger family, and curcumin is the active ingredient that gives it that yellowish color. It has been used in Ayurvedic and Chinese medicine for over 2,000 years, and there are now enough studies in major depression to support a meta-analysis. Two recent such analyses found 10 studies that met the Cochrane criteria. They concluded that curcumin had an effect size comparable to standard antidepressants—in the small to medium range (0.3–0.7). It has also gone head to head against SSRIs and those trials found similar efficacy (Wang Z et al, J Affect Disord 2021;282:242–251; Fusar-Poli L et al, Crit Rev Food Sci Nutr 2020;60(15):2643–2653).
TCPR: How does it work?
Dr. Mendelson: The mechanism is unclear. Curcumin is not a flavonoid, but like the flavonoids it has very potent antioxidant, anti-inflammatory, and neuroprotective effects. For example, it increases brain-derived neurotrophic factor (BDNF) and reduces the inflammatory cytokines, tumor necrosis factor, and interleukin 1-beta. Like the adaptogens, it also reduces serum cortisol.
TCPR: Does turmeric (curcumin) have other benefits?
Dr. Mendelson: It improves cognition, particularly working memory. There are about eight small, randomized controlled trials showing cognitive benefits with curcumin in various populations, and the clearest signal is in older adults (Tsai IC et al, Pharmaceuticals (Basel) 2021;14(12):1235). As an anti-inflammatory, it also improves various types of arthritis, including osteoarthritis, rheumatoid arthritis, and gout (Zhu LN et al, Phytother Res 2019;33(3):524–533; Zeng L et al, Front Immunol 2022;13:891822).
TCPR: Any tips on purchasing curcumin?
Dr. Mendelson: Most of the research used products with 95% curcuminoids. I’d also look for curcumin products that contain piperine. This is an extract of black pepper that enhances the absorption of curcumin and other phytochemicals. That’s important because otherwise curcumin has very low bioavailability.
TCPR: Any risks with curcumin?
Dr. Mendelson: Overall it is well tolerated. It has mild anticoagulant effects, so you might be cautious in patients who are taking an anticoagulant. Unlike St. John’s wort, it does not affect the monoamines, so in theory it should not cause mania. It did reduce mania in an animal model, and there are no reports of mania on curcumin in the literature (Gazal M et al, Eur J Pharmacol 2014;724:132–139).
TCPR: The third herb you mentioned was saffron. Tell us a little about that.
Dr. Mendelson: Like curcumin, saffron has anti-inflammatory, antioxidant, and neurotrophic effects and a long history of use in Chinese and Ayurvedic medicine. The modern studies began in 2004, and about 17 small, randomized controlled trials have tested it in mild to moderate depression since then. It worked as monotherapy and as augmentation. In six of those trials it was compared head to head with an SSRI or tricyclic, and saffron worked just as well. Most of the studies came from a single group in Iran, but that work has been validated by independent groups (Musazadeh V et al, Pharmacol Res 2022;175:105963).
TCPR: How do you find a good saffron product?
Dr. Mendelson: Most of the studies dosed it at 15 mg BID, but there was a lot of variation in what those capsules contained. Some used 2% safranal (0.3 mg of safranal per 15 mg), but that dose is hard to come by as most products contain 3%. Some used a combined extract of 0.15 mg safranal and 0.7 mg crocin per 15 mg. Some extracted it from the petal, and others from the stigma. A few studies used proprietary extracts like Satiereal, which is available from Life Extension and is dosed differently—at 176.5 mg because it contains a lower percentage of safranal (0.3%). As far as we can tell, all these products work equally well (Lopresti AL and Drummond PD, Hum Psychopharmacol 2014;29(6):517–527).
TCPR: Does saffron have other benefits?
Dr. Mendelson: There are small studies in anxiety, OCD, ADHD, weight loss, premenstrual symptoms, and male and female sexual dysfunction, but most of those findings have not been replicated, so I would take them with a grain of salt.
TCPR: Any risks with saffron?
Dr. Mendelson: It is well tolerated, with possible GI side effects. Like curcumin, it has some anticoagulant effects, but otherwise no serious risks have shown up for this herb.
TCPR: When would you suggest we use herbal therapies?
Dr. Mendelson: I am not a champion of herbal treatment. I am simply a champion of expanding our pharmacological repertoire, and herbs can be helpful. Some patients prefer the herbal approach, and it is important to have enough knowledge about herbs to accommodate them. Other patients don’t tolerate standard treatments well, and many are happy to learn that there are herbal alternatives that don’t tend to cause drowsiness, sexual side effects, or weight gain. Then there are those who do not respond to standard treatments, and—with the exception of St. John’s wort—most herbs can be safely added in as augmentation.
TCPR: When would you avoid them?
Dr. Mendelson: In severe illness. Most of the clinical studies of herbal treatments have evaluated only mild to moderate forms of psychiatric illness.
TCPR: Thank you for your time, Dr. Mendelson.
Newsletters
Please see our Terms and Conditions, Privacy Policy, Subscription Agreement, Use of Cookies, and Hardware/Software Requirements to view our website.
© 2026 Carlat Publishing, LLC and Affiliates, All Rights Reserved.


_-The-Breakthrough-Antipsychotic-That-Could-Change-Everything.webp?t=1729528747)



