Intravenous Buprenorphine Microinduction
Marissa Bayerl, APRN, and Noah Capurso, MD, MHS. Ms. Bayerl and Dr. Capurso have no financial relationships with companies related to this material.
REVIEW OF: Jablonski LA et al, Drug Alcohol Depend 2022;237:109541
STUDY TYPE: Retrospective chart review
Buprenorphine (BUP) is a lifesaving first-line treatment for opioid use disorder (OUD), but the process of starting it, called induction, can be tricky due to the possibility of precipitated withdrawal. Various strategies have been developed to get around this. One of the most promising, called microinduction, introduces very low doses while the patient still has opioids in their system, and the dose of BUP is then escalated (see CATR November/December 2021).
The small doses required for microinduction can be challenging to obtain and administer. Cutting tablets into fractions smaller than halves can be inconsistent, and although widely practiced, cutting films into smaller fractions is unreliable as well (Reindel KL et al, Int J Pharm Compd 2019;23(3):258–263). Certain health care systems may not carry formulations that can be easily subdivided. Transdermal patches and buccal films can be utilized, but these may not always be available either.
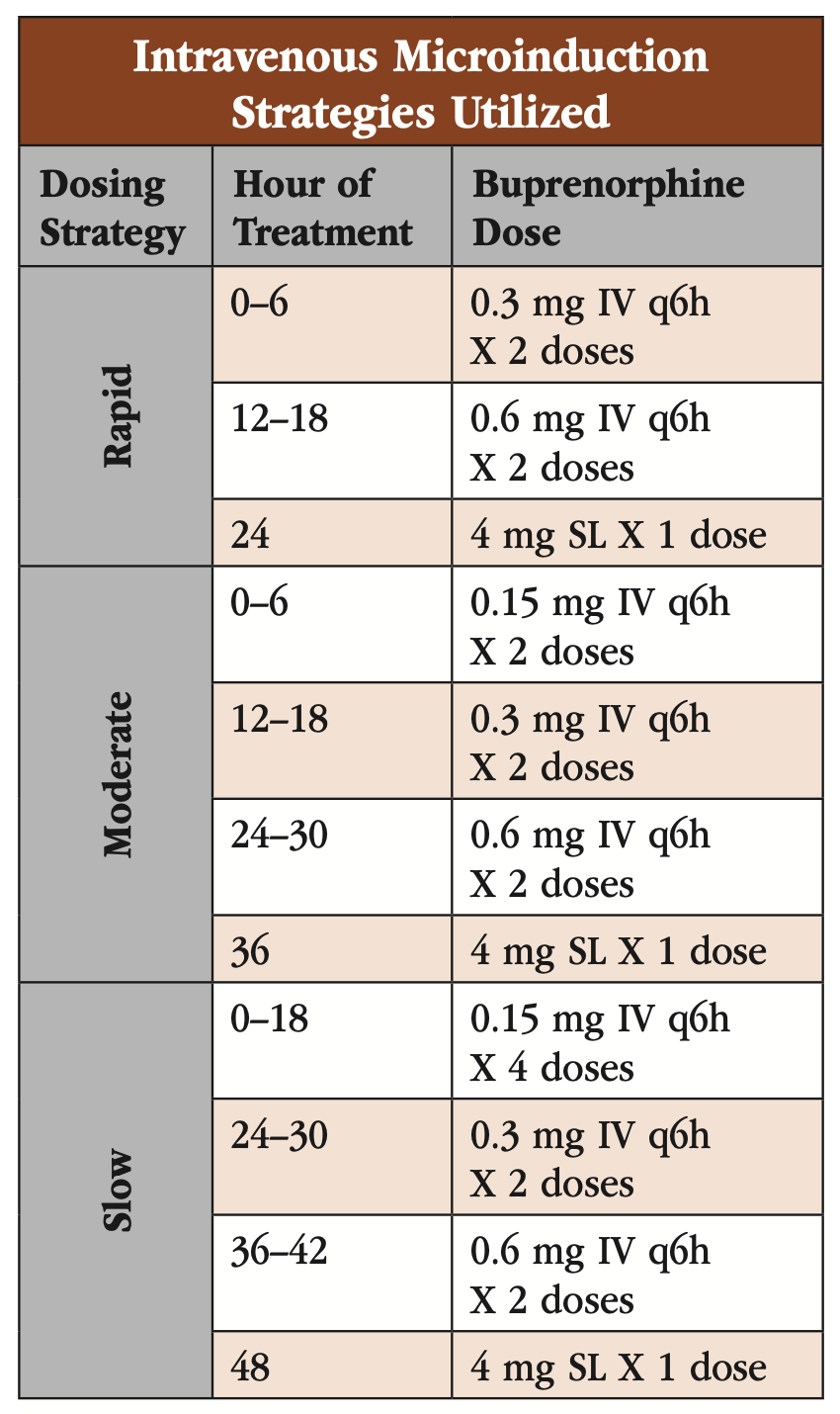
Researchers therefore sought to create a reliable microinduction protocol for patients hospitalized on medical floors utilizing intravenous BUP (IV-BUP), which is inexpensive and easy to dose in small increments (see “Intravenous Microinduction Strategies Utilized” table). They made the doses available to clinicians in a large academic hospital. After six months, the researchers performed a retrospective chart review in order to determine feasibility and tolerability.
They identified 59 cases: 34 (58%) were female, the median age was 52, and the median duration of OUD diagnosis was 20 years. 54 (91.5%) of the patients completed the protocol, with 44 (74.6%) of them being fully adherent. The IV-BUP microinduction strategy was well tolerated; nearly three-quarters had Clinical Opiate Withdrawal Scale (COWS) scores that remained below 8, and none of the remaining patients had a score above 12 (anything ≤12 is considered mild). Rates of protocol completion, tolerability, frequency of deviation, and COWS scores were similar across the three protocols, though clinicians chose the moderate and slow strategies when converting from methadone.
The numbers here are relatively small, and the choice of protocol was not randomized or blinded. But the high percentage of completions, low number of protocol deviations, and low COWS scores suggest that IV-BUP microinduction is feasible and well tolerated, at least on medical floors of a large academic hospital. The authors point out that previously published microinductions typically took four or more days to complete, whereas this approach takes only 24–48 hours, another potential advantage.
CARLAT TAKE
Microinduction is a way to start BUP while minimizing the risk of precipitated withdrawal. Sublingual and transdermal protocols have already been developed, and this study shows that small intravenous doses can work as well. This is a small study, but you can consider this approach for medically hospitalized patients if small sublingual or transdermal doses are unavailable.

Newsletters
Please see our Terms and Conditions, Privacy Policy, Subscription Agreement, Use of Cookies, and Hardware/Software Requirements to view our website.
© 2026 Carlat Publishing, LLC and Affiliates, All Rights Reserved.


_-The-Breakthrough-Antipsychotic-That-Could-Change-Everything.webp?t=1729528747)



