Home » Smartphone Apps as Adjuncts for Substance Use Treatment
Smartphone Apps as Adjuncts for Substance Use Treatment
December 10, 2020
From The Carlat Addiction Treatment Report
Rehan Aziz, MD.
Associate Professor of Psychiatry and Neurology, Rutgers Robert Wood Johnson Medical School.
Dr. Aziz has disclosed that he has no relevant financial or other interests in any commercial companies pertaining to this educational activity.
The majority (81%) of Americans own a smartphone, and a little over one-half (58%) have downloaded a health-related app (www.pewresearch.org/internet/fact-sheet/mobile). Could addiction apps be the next tool to improve treatment outcomes? This article will review some apps for substance use disorders (SUD) and discuss strategies for integrating them into your practice.
FDA-cleared apps for treatment
There are two mobile apps that have received FDA clearance for inclusion in SUD treatment paradigms: reSET and reSET-O. They are available for anyone to download, but in order to use them, patients need to enter an access code. They get the code when their providers enroll them with the app developer, Pear Therapeutics (www.resetforrecovery.com). Cost and insurance coverage for the apps may be a limiting factor for some patients.
reSET
reSET is a 90-day package that provides cognitive behavioral therapy (CBT) as an adjunct to contingency management (CM). It’s for English-speaking patients 18 and older who are in outpatient treatment. The app has 61 CBT-based education modules, which patients complete 3 to 4 times a week. Clinicians can monitor patients’ progress via a dashboard that includes lessons completed, reported substance use, reported cravings and triggers, and compliance rewards. Clinicians can also input urine drug screen results.
FDA requirements aren’t as stringent for apps as for medications. reSET was cleared based on a multisite, unblinded 12-week trial of 399 patients who received either standard treatment or standard treatment plus reSET on a desktop computer, not a smartphone. The data showed a statistically significant increase in adherence to abstinence for patients with alcohol, cocaine, marijuana, and stimulant use disorders in those who used reSET compared to those who didn’t: 40.3% vs 17.6% (www.fda.gov/news-events/press-announcements/fda-permits-marketing-mobile-medical-application-substance-use-disorder).
reSET-O
reSET-O is an 84-day program for opioid use disorder (OUD) that’s intended to increase retention of patients in outpatient treatment by providing CBT, as an adjunct to treatment that includes transmucosal buprenorphine and CM.
For its clearance, the FDA reviewed data from a multisite, unblinded, controlled 12-week trial of 170 patients who received supervised buprenorphine treatment paired with a behavior therapy program, either with or without reSET-O. The use of reSET-O didn’t decrease illicit drug use more than standard treatment. However, the data showed a statistically significant increase in treatment retention for the 12 weeks over which patients used reSET-O compared to those who didn’t: 82.4% vs 68.4% (www.fda.gov/news-events/press-announcements/fda-clears-mobile-medical-app-help-those-opioid-use-disorder-stay-recovery-programs).
Overall, the data for these apps aren’t too impressive given that reSET-O didn’t help patients maintain abstinence and both apps were tested in unblinded conditions. Both also use CM, a rewards-based therapy. This may make them difficult for practitioners to adopt.
Additional apps for treatment (not FDA cleared)
In a recent study, researchers conducted a systematic search of the iTunes and Google Play app stores for free or low-cost addiction apps. They found that as of March 2018, there were 904 apps targeting SUDs. Most of these apps were eliminated from further analysis for a variety of reasons, including having no user ratings, being primarily music or gaming apps, costing more than $1, or being based solely on the 12-step model. (Ed note: Apps based on the 12-step model were not reviewed because of the large quantity of apps and limited study resources and lack of content pertaining to medications for addiction treatment and effective behavior change models outlined by federal and expert guidelines.)
Of the 74 apps remaining, most scored low on the Mobile App Rating Scale (MARS) for engagement, functionality, aesthetics, information, and satisfaction. Few apps integrated evidence-based psychotherapies or pharmacologic interventions. Some apps even allowed other users to promote harmful drinking and drug use (Tofighi B et al, JMIR Mhealth Uhealth 2019;7(4):e11831).
Advantages and disadvantages
Apps have several pluses. They are readily available and work through devices that most people keep nearby. They can increase access to evidence-based interventions, like CBT, CM, and psychoeducation. Many are obtainable at little or no cost. They can decrease stigma involved in seeking care. They can also be safely used during a time of physical distancing.
However, most apps lack research support, so we don’t know if they actually improve patient outcomes. While most Americans have downloaded a health app at one point or other, almost half (46%) discontinue using them. Reasons for stopping include high data entry burden, loss of interest, concerns with data-collection accuracy, and costs. Patients most amenable to health apps have tended to be younger, have higher incomes, be more educated, and be Latino/Hispanic (Krebs P et al, JMIR Mhealth Uhealth 2015;3(4):e101).
Adding apps to your practice
Apps work best as an adjunct to established treatment and in the context of a strong therapeutic alliance. I would start by asking your patients if they have tried any addiction apps on their own. Chances are they have. Then ask what their experience was and what features were most important to them. Familiarize yourself with a few apps that you can discuss. For patients interested in trying an app, make sure to emphasize that apps are a useful tool but not a substitute for therapy and medications. Let them know that apps can contain false information. Take time to review patients’ use of apps during sessions and address questions or confusion they may have.
CATR Verdict: If properly vetted, addiction apps can be a useful, though largely untested, adjunct to established addiction treatment. Clinicians should ask patients about their app use and discuss pros and cons of apps with them.
Addiction TreatmentFDA-cleared apps for treatment
There are two mobile apps that have received FDA clearance for inclusion in SUD treatment paradigms: reSET and reSET-O. They are available for anyone to download, but in order to use them, patients need to enter an access code. They get the code when their providers enroll them with the app developer, Pear Therapeutics (www.resetforrecovery.com). Cost and insurance coverage for the apps may be a limiting factor for some patients.
Table: FDA-Cleared Apps for Substance Use Treatment
(Click to view full-sized PDF.)
reSET
reSET is a 90-day package that provides cognitive behavioral therapy (CBT) as an adjunct to contingency management (CM). It’s for English-speaking patients 18 and older who are in outpatient treatment. The app has 61 CBT-based education modules, which patients complete 3 to 4 times a week. Clinicians can monitor patients’ progress via a dashboard that includes lessons completed, reported substance use, reported cravings and triggers, and compliance rewards. Clinicians can also input urine drug screen results.
FDA requirements aren’t as stringent for apps as for medications. reSET was cleared based on a multisite, unblinded 12-week trial of 399 patients who received either standard treatment or standard treatment plus reSET on a desktop computer, not a smartphone. The data showed a statistically significant increase in adherence to abstinence for patients with alcohol, cocaine, marijuana, and stimulant use disorders in those who used reSET compared to those who didn’t: 40.3% vs 17.6% (www.fda.gov/news-events/press-announcements/fda-permits-marketing-mobile-medical-application-substance-use-disorder).
reSET-O
reSET-O is an 84-day program for opioid use disorder (OUD) that’s intended to increase retention of patients in outpatient treatment by providing CBT, as an adjunct to treatment that includes transmucosal buprenorphine and CM.
For its clearance, the FDA reviewed data from a multisite, unblinded, controlled 12-week trial of 170 patients who received supervised buprenorphine treatment paired with a behavior therapy program, either with or without reSET-O. The use of reSET-O didn’t decrease illicit drug use more than standard treatment. However, the data showed a statistically significant increase in treatment retention for the 12 weeks over which patients used reSET-O compared to those who didn’t: 82.4% vs 68.4% (www.fda.gov/news-events/press-announcements/fda-clears-mobile-medical-app-help-those-opioid-use-disorder-stay-recovery-programs).
Overall, the data for these apps aren’t too impressive given that reSET-O didn’t help patients maintain abstinence and both apps were tested in unblinded conditions. Both also use CM, a rewards-based therapy. This may make them difficult for practitioners to adopt.
Additional apps for treatment (not FDA cleared)
In a recent study, researchers conducted a systematic search of the iTunes and Google Play app stores for free or low-cost addiction apps. They found that as of March 2018, there were 904 apps targeting SUDs. Most of these apps were eliminated from further analysis for a variety of reasons, including having no user ratings, being primarily music or gaming apps, costing more than $1, or being based solely on the 12-step model. (Ed note: Apps based on the 12-step model were not reviewed because of the large quantity of apps and limited study resources and lack of content pertaining to medications for addiction treatment and effective behavior change models outlined by federal and expert guidelines.)
Of the 74 apps remaining, most scored low on the Mobile App Rating Scale (MARS) for engagement, functionality, aesthetics, information, and satisfaction. Few apps integrated evidence-based psychotherapies or pharmacologic interventions. Some apps even allowed other users to promote harmful drinking and drug use (Tofighi B et al, JMIR Mhealth Uhealth 2019;7(4):e11831).
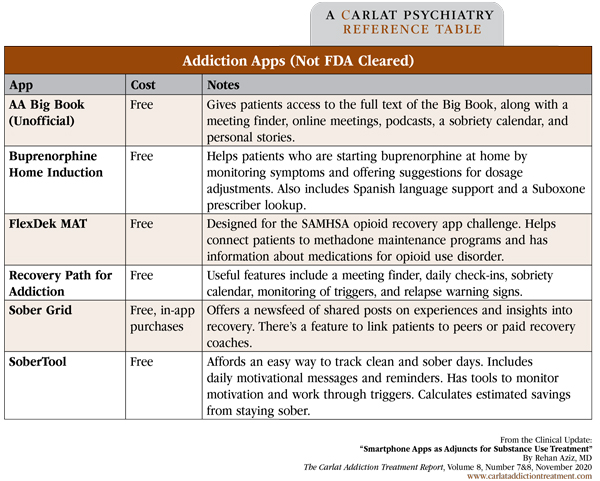
Table: Addiction Apps (Not FDA Cleared)
(Click to view full-sized PDF.)
Advantages and disadvantages
Apps have several pluses. They are readily available and work through devices that most people keep nearby. They can increase access to evidence-based interventions, like CBT, CM, and psychoeducation. Many are obtainable at little or no cost. They can decrease stigma involved in seeking care. They can also be safely used during a time of physical distancing.
However, most apps lack research support, so we don’t know if they actually improve patient outcomes. While most Americans have downloaded a health app at one point or other, almost half (46%) discontinue using them. Reasons for stopping include high data entry burden, loss of interest, concerns with data-collection accuracy, and costs. Patients most amenable to health apps have tended to be younger, have higher incomes, be more educated, and be Latino/Hispanic (Krebs P et al, JMIR Mhealth Uhealth 2015;3(4):e101).
Adding apps to your practice
Apps work best as an adjunct to established treatment and in the context of a strong therapeutic alliance. I would start by asking your patients if they have tried any addiction apps on their own. Chances are they have. Then ask what their experience was and what features were most important to them. Familiarize yourself with a few apps that you can discuss. For patients interested in trying an app, make sure to emphasize that apps are a useful tool but not a substitute for therapy and medications. Let them know that apps can contain false information. Take time to review patients’ use of apps during sessions and address questions or confusion they may have.
CATR Verdict: If properly vetted, addiction apps can be a useful, though largely untested, adjunct to established addiction treatment. Clinicians should ask patients about their app use and discuss pros and cons of apps with them.
KEYWORDS addiction-treatment behavioral-therapy complementary-treatments computers_in_psychiatric_practice electronic-use health-apps internet media telehealth telemedicine
Issue Date: December 10, 2020
Table Of Contents
Recommended
Newsletters
Please see our Terms and Conditions, Privacy Policy, Subscription Agreement, Use of Cookies, and Hardware/Software Requirements to view our website.
© 2026 Carlat Publishing, LLC and Affiliates, All Rights Reserved.



_-The-Breakthrough-Antipsychotic-That-Could-Change-Everything.webp?t=1729528747)



